I’m finally getting to the ‘run’ stage of my breast cancer triathlon swim/bike/run analogy – radiotherapy. Many women who have a mastectomy don’t need radiotherapy. It’s always given to women who have a lumpectomy, to treat the breast tissue that is left behind. In my case, because my tumour was large (131mm) and I had 3 positive lymph nodes, radiotherapy was added on after chemotherapy and surgery.
I’m getting radiotherapy to the chest wall, as the deep margin of my mastectomy specimen was positive. I’m also getting it to my supraclavicular fossa (the lymph nodes above your collar bone), because I had positive axillary nodes. I’m also getting it to my internal mammary chain – the lymph nodes just behind your breastbone, because of the size of my tumour.
Raise your hands
Ideally radiotherapy is given within 4-6 weeks after your surgery, but some women have delays because they need a second operation, or have problems with wound healing. Mine was delayed because I had to wait for my nipple scab to fall off and the skin underneath to heal properly and because I had to be able to get both arms above my head for both the planning scan and the treatment.
The nipple full healed after 7 weeks following my mastectomy but because of the cording that I’ve talked about before, I couldn’t get my arm above my head. I found a great physiotherapist, Katrina Wade at Bodyworks Physiotherapy Clinic in Colchester, who got my arm moving in 2 sessions, which was a huge relief. I’m now planning on creating a database of physiotherapists who are trained in releasing cording, to make it easier for patients like me to get the treatment they need.
Planning scan
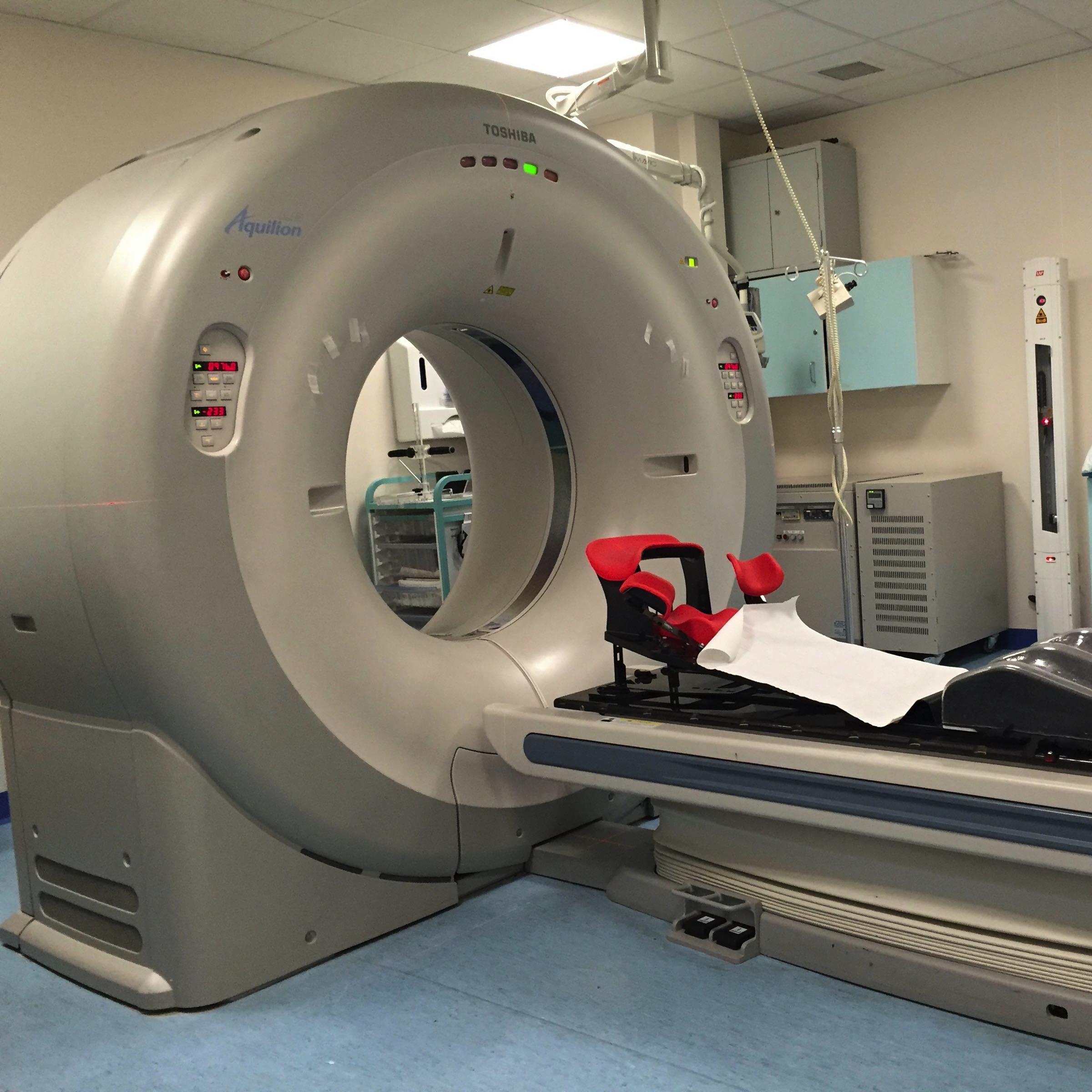
Before the radiotherapy starts, you have a planning CT scan to map out which areas to target. My radiotherapy is being done at Addenbrookes, which makes for a 3 hour round trip. I found the planning CT scan surprisingly emotional. It was the fear of the unknown that got me – sitting in a waiting room by yourself and not knowing what was going to happen. The whole process took about 20 minutes. I had to lie on a narrow bed with both arms above my head, and be still. I went into and out of the scanner, whilst images were taken. They taped a thin wire over my scar so they could see where it was on the screen, and drew 3 crosses on the middle of my chest and both sides, where the tattoos would go.
The room itself was cold, thanks to the air conditioning needed to keep the CT scanner running. I stripped to the waist, and then walked about 5 metres to the scanner. They offered me a gown to put on, which I would then keep and wear for all my radiotherapy sessions, but I didn’t see the point of wearing it for all of 10 seconds.
It did feel quite emotional, lying half naked in a room with technicians wandering in and out. They put a blanket over my legs to keep me warm, and eventually the scan was done. All that was left to do was tattoo me. The tattoos are tiny black dots that look like blackheads. They are used to put you in exactly the same position for every treatment. I didn’t feel the ones on my left hand side and the centre of my chest (numb following the surgery) but the right-hand one was a sharp scratch, like having blood taken.
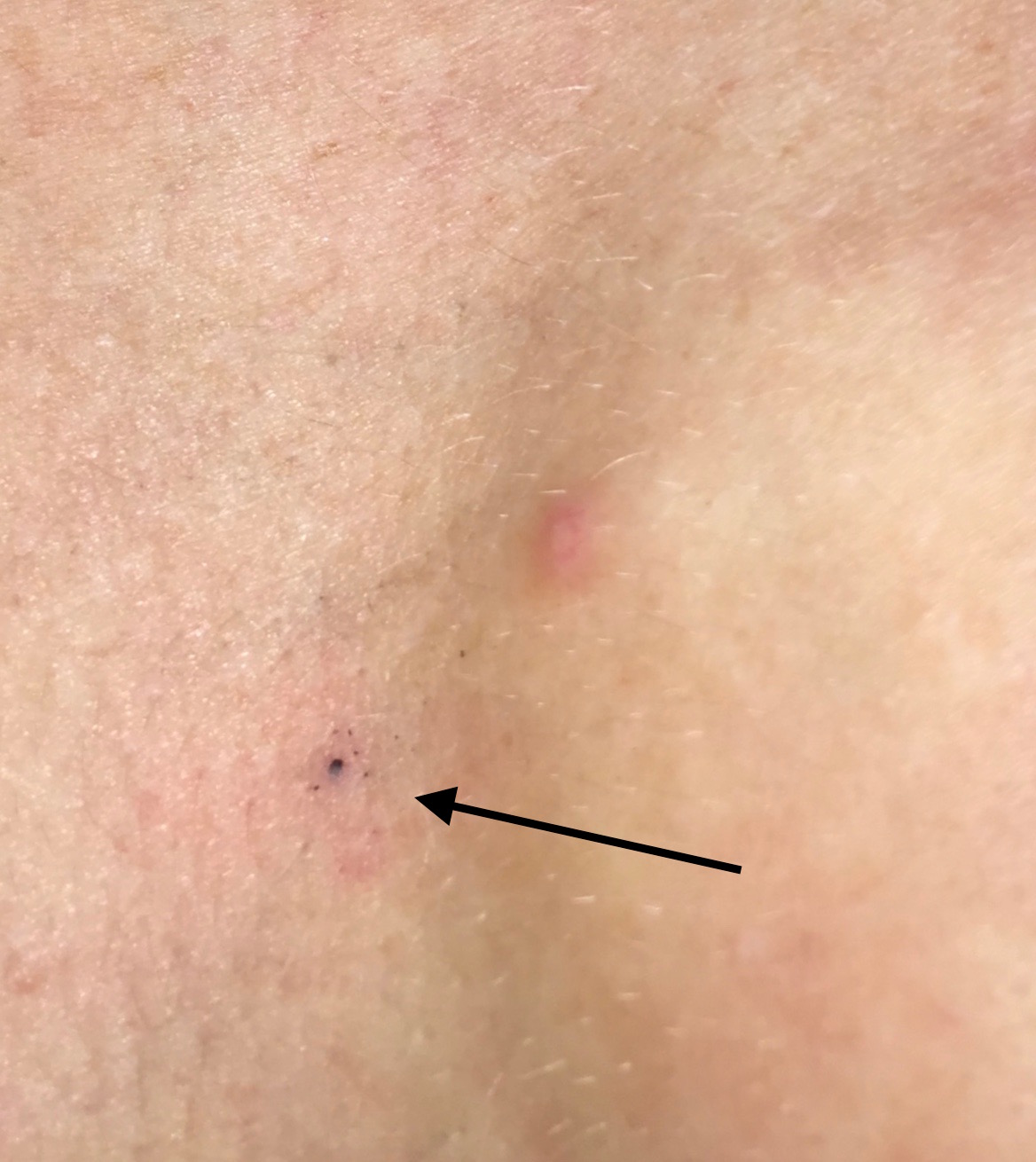
Tattoo on my breastbone
They also took a photograph of my face, to confirm my identity at every treatment, and a photo of the way my hands and arms were positioned, again to help get me in the exact position every time.
What to expect
I was told that it would take 1-2 weeks to notice any skin changes. I have seen patients with severe skin reactions (burns, blisters, discolouration) and those who have had nothing. There doesn’t seem to be any reason why one woman gets side-effects and another doesn’t. It’s just luck of the draw. Another thing that could happen is that my implant will develop a capsule around it, which can contract down and make the implant look and feel like a hard tennis ball. Nice. Again, there’s no way of predicting who this will happen to. The Strattice mesh that we use during implant surgery is thought to provide some protection from this.
This guide from Breast Cancer Care goes through all the possible side-effects of radiotherapy.
I was told that I might feel tired after radiotherapy, and that this would peak at about 6 weeks after treatment. I’m still getting used to feeling absolutely knackered if I have a busy 3-4 days, and the thought of being even more tired was not great. Patients had told me before that they were exhausted after radiotherapy, but I had never understood why. Now, having had my body battered by chemo and 2 operations, I’m beginning to understand how draining all these treatments can be. Especially when you have a 3 hour round trip every day, Monday-Friday, for 3 weeks, to get the treatment.
I was advised to use a simple emollient cream like E45 and to use a natural roll-on deodorant, not to shave the hair under my arms and that if blisters did develop I would be given dressings. I was also told to wear a cotton bra or even go braless afterwards.
Time to get zapped
Three weeks later, my radiotherapy started. I had my time slots for the 3 weeks given to me, with a 4-day break for Easter. The room was even colder than the scanning room. I had a male and a female radiotherapist, and I just had to get over the little bit of modesty I had left, strip off and get on with it.
I lay down on the bed and it took a couple of minutes to line my tattoos with the lasers. Then I had a CT scan to check the position was accurate. After a couple of minutes, the radiotherapy itself started. I was slowly moved into the machine whilst the treatment took place. It was a bit of an anti-climax. I was expecting lights and whistles and bells – instead I got to look at stickers that had been stuck on the inside of the machine, and listen to the noise.
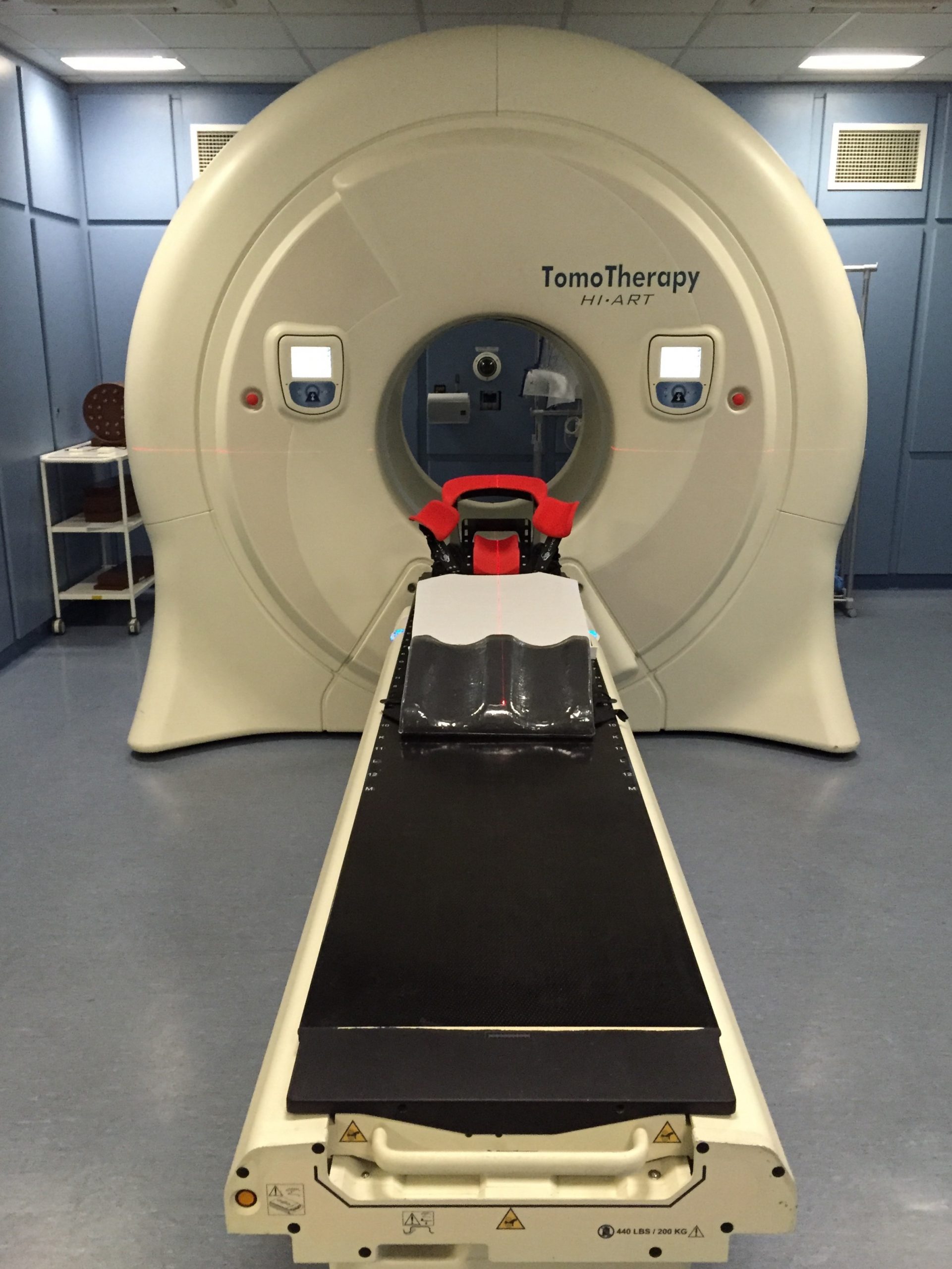
Radiotherapy machine
Have you ever sat and listened to mice scuttling around in the loft overhead? Well, radiotherapy sounded (to me) like giant mice pushing a shopping trolley on gravel. A grinding noise that moves from left to right following the radiotherapy beams, somewhere between a CT and an MRI in volume.
At the end of the treatment, my arms had gone numb. Partly from the cold and partly from being left in that position for so long, which I’m not used to. My treatment took longer than most women, because I’m having 3 areas treated. I had to ask the radiotherapist to bring my arms down for me!
Tips
I took a photo of my breasts before treatment started, so I can monitor any skin changes and I’m being a bit anally retentive and doing this every day. Although when I show people other photos on my phone (such as the amazing chocolate Cumberbunny that Dermot got me for Easter from Chocolatician), it’s a bit awkward having to whizz past my topless shots which they really don’t need to see.

I took my cycling arm warmers with me to the next 2 sessions and wore a pair of gloves which made a world of difference. I also thought – if you find the room cold and don’t have arm warmers (as most women wouldn’t), an old pair of wooly tights or leggings cut in half would do the job as well.
Someone told me about R1 and R2 Waterjel which are available on prescription, and are meant to protect the skin against radiotherapy damage. One has to be applied as soon after treatment as possible, and then let your breasts air-dry, and the other is applied 2-3 times a day as a moisturiser. I’ve not bothered investigating this, as I can’t exactly walk to the park and ride topless or drive home topless in my car. But if your radiotherapy treatment was closer to home, it might be worth asking your GP about this.
I’ve got 13 sessions left, and I’m curious to know what will happen to my skin and my implant. Watch this space. I’d also love to hear any tips or tricks for surviving radiotherapy from those of you who’ve been through it before me.