So today was Day 8, the start of week 2. And it didn’t start well. I woke up silently screaming at 1am with the worst headache I have ever, ever had. I was crying with the pain. Paracetamol and ibuprofen didn’t touch it. I didn’t want to wake my husband, as he was about to start a 3-day weekend on-call as the consultant surgeon, so I lay there, in the dark, waiting for the sun to rise.
I eventually drifted off to sleep, only to wake up from a horrific nightmare. I dreamt that I was being chased, raped and then buried alive. I knew chemotherapy could give you headaches but nightmares…? Lets just say I was very glad when my alarm went off at 6am for my morning walk with my neighbour.
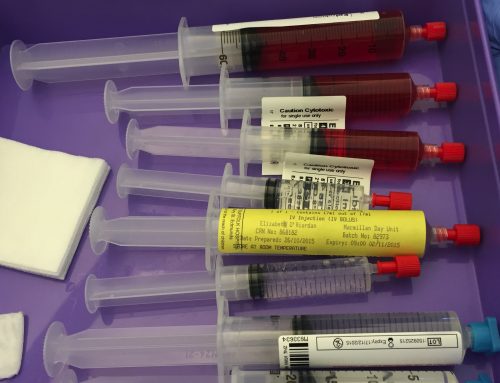
Week 2 tablets
I then went back to bed and managed to sleep through until 10, which was a blessing. I physically felt a bit brighter, and the chemo fog was starting to lift, but the headache was unbearable. On top of the final injection today, I also started a week of Augmentin (antibiotic – also known as co-amoxiclav) and fluconazole (anti-fungal). The second week is when my neutrophil count can drop to very low levels meaning I can pick up any infection going, so most chemotherapy patients are given antibiotics to prevent this. You’re also meant to stay away from anyone with a cough or cold.
Ringing for advice

I finally had the common sense to ring my oncology specialist nurse for advice about the headaches. As a doctor, I am very good at coping with illness by myself. A little bit of ‘Physician, Heal Thyself’, and a lot of not wanting to bother anyone. Plus, I knew chemo was meant to make you feel like shit – so why ring anyone to tell them that yes, you do feel like shit.
The nurse was very helpful, and suggested that the headaches could be due to the daily G-CSF injections, and I could have some stronger painkillers for the next cycle of chemo. I took my temperature during the day, and it was low (35.2C). I was also feeling shivery and rotten. I knew that having a high temp (well, high for chemo patients) of over 37.5 C was a danger sign but no-one had said anything about having a low temperature. As a doctor, a low temperature is just as worrying as a high one, and if a patient of mine had a temperature of 35C, I would be worried.
Time to go to the day unit
I checked my temperature again during the day, and it was still reading 35.2C, so I rang the nurse again. She said that I had better come in to the day unit to get my bloods checked, and to bring an overnight bag, just in case. Mild panic – that chemo bag that I had told myself I would pack…well…. errmmmmm….. This is what I packed in a hurry.
Chemo overnight bag
- pyjamas (I have a dressing gown ready for when it’s cold)
- underwear
- change of clothes
- warm socks
- slippers
- iPhone charger (very important)
- small wallet with £40 and one debit card (rather than my normal purse)
- chemo cuddly toy from my parents
- notepad and pen
- Robinson Barley Water squash
- all my tablets and the final GCSF injection
- toothbrush, Biotin toothpaste and Difflam mouthwash
- travel shower gel and face wash
- hand cream and lip salve
- fleecy throw
- biscuits to snack on
- A pillow (Kate Granger had told me that hospital pillows are awful so I put a pillow in the car just in case. An alternative is to take a nice pillow case)
I drove in, and this maybe wasn’t the most sensible thing I have ever done. It’s only 20 minutes, but I was feeling a little wobbly, especially as I hadn’t eaten lunch, and it was the first time I had driven since the chemo. I think adrenaline has a lot to answer for, and I wasn’t thinking sensibly.
The Day Unit
The chemo nurse Lynsey was amazing. I was seen in their new treatment room, and got to sit in the fab reclining chemo chair again. She took bloods and cultures from my port, and cultures from the back of my hand, and gave me some antibiotics (Tazocin or piperacillin/tazobactam) through the port. She also gave me some codeine for my headache, which worked within about 30 minutes – such a relief!
My temperature was 36.4C in the day unit, which showed how inaccurate my home thermometer was. How do you know if your thermometer at home is reading properly? I forgot to take mine with me to double-check, but when I buy a new one, I will make sure it goes with me, if there is a next time. You can get quite obsessed about thermometers and checking temps! Luckily, all the bloods were normal, and by the time my husband had come out of his afternoon meeting, I was all set for him to drive me home.
Sepsis
Now it’s time for a bit of a rant about not educating patients properly. Sepsis is dangerous, and especially dangerous in chemotherapy patients whose immune system has been compromised. There has been a massive campaign introduced recently to improve the management and treatment of sepsis, and prevent unnecessary early deaths. For more details on the treatment of sepsis see The UK Sepsis Trust ( for patients) and The RCP Sepsis Tool Kit (for health professionals).
Basically, it’s been made really simple, as the ‘Sepsis Six’. Doctors and nurses should measure 3 things:
- Serum lactate and send full blood count
- Urine output
- Blood cultures
And then do 3 things:
- Give iv antibiotics
- Start iv fluids
- Give high flow oxygen
Now, I know as a doctor that it is vital that antibiotics are given within the first hour of admission / being seen in A&E, in anyone showing signs of sepsis, without waiting for the results of blood tests and X-rays or a senior review. A nurse should be able to follow the protocol and get a doctor to prescribe the antibiotics on a drug chart, if a patient is septic, to get things done within the golden hour.
In England, there is a national CQUIN bonus payment to meet the Acute Oncology Service standards, including giving IV antibiotics within 60 minutes. This, along with the other 5 steps, saves lives.
Lack of patient education

When I started my journey as a chemo patient, all I was told that if my temperature was above 37.5C, I needed to go in to hospital to be assessed. I was given a small credit-card sized piece of paper with a bleep on it. A friend of mine going through chemo at the same time as me in a different hospital was given an A4 sheet of traffic-light warnings telling her what to do for each symptom she might have, and what needed to be taken seriously. There is a massive difference in the amount of information given to cancer patients. We quickly become experts in our own illness, or our family do on our behalf, and the more information we have, the better we can prepare ourselves.
I strongly believe we need to educate patients properly. During the day, if you are seen by an oncology nurse in a chemo day unit, then you will have prompt treatment. But if you have to go in out-of-hours, there’s a chance that the doctor or nurse admitting you won’t be familiar with the sepsis protocol.
By telling patients that they should expect (and if necessary demand) to be given antibiotics within an hour of admission, it does three things:
- It makes them go to hospital quickly, rather than faffing about at home for a few hours. The longer it takes them to get to hospital, the longer it takes to get the antibiotics in.
- They can tell the doctor or nurse admitting them that they are meant to have antibiotics within the hour.
- It empowers the patient.
Later that night
Rant over. That night I perked up a bit, and managed to almost taste my evening meal. Before I went to bed I weighed myself, out of interest. I was shocked to see that I had lost 3.5kg within the week – not what the oncologist and my breast surgeon had ordered.
I added some laxatives to the tablet mix as I hadn’t been for a few days and was worried about getting constipated. I was glad to give myself the final injection. With the headache finally gone, I hoped I would get a bit of sleep tonight.