The time had come. After months of indecision about what type of mastectomy I wanted, it was time to go to hospital. The alarm went off at the crack of dawn and Dermot and I nervously got up and got dressed. We were both ready for the bike leg of my breast cancer triathlon.
Gin and Tonic, anyone?
I had to stop eating at midnight, and could drink clear fluids until 6.30am. My wonderful brother got me a gin advent calendar, now that my taste had come back. And as gin and tonic is clear, surely it would be OK to have one before my surgery…? No-one had told me that I couldn’t have alcohol on the morning of my surgery. Of course, I was far too sensible, but in the midst of sorting out the dogs and ducks before we set off to be at the hospital at 7, I forgot to drink much of anything, and was very thirsty when I arrived.

Final prep
I got ushered into a side room, and all the nurses were wonderful – treating me as Liz, not Liz the doctor or Liz, Dermot’s wife. In no time at all I was stripped, in my theatre gown with my lovely green TED stockings on, waiting for people to arrive. I was allowed to sip water, which I was really grateful for. A student nurse gave me some meal cards to fill in, but I didn’t have a pen, so had to press the buzzer to get someone to bring me one.
The anaesthetist was wonderful. She put me at ease, and said she would put a local anaesthetic block in to numb my pectoral muscle after the surgery. It was a bit scary being reminded of all the potential complications, such as puncturing my lung. I say scary things like this to my patients all the time, knowing that the chance of it happening is actually very small. However, hearing someone say it to me, and realising that it might happen to me, was very different.
I had one request, and asked that they be careful when they pulled the tape off my eyes when I was waking up, so I could hang on to my few remaining eyelashes. Your eyes are normally taped shut when you have a general anaesthetic. She said they would make sure no eyelashes were harmed, and would use a gel pad instead. It’s funny how little things such as keeping my remaining five eyelashes was suddenly so important to me.
Art Class
The last person to see me was my surgeon, who went over the consent again. She reminded me that I would have blue urine (due to the dye used to help with the armpit lymph node surgery) but I was zoning out when she went over the rest of the details. I was nervous and scared but trying to be brave, to help her as well as me, and just wanted to get things over with. She then drew on me.
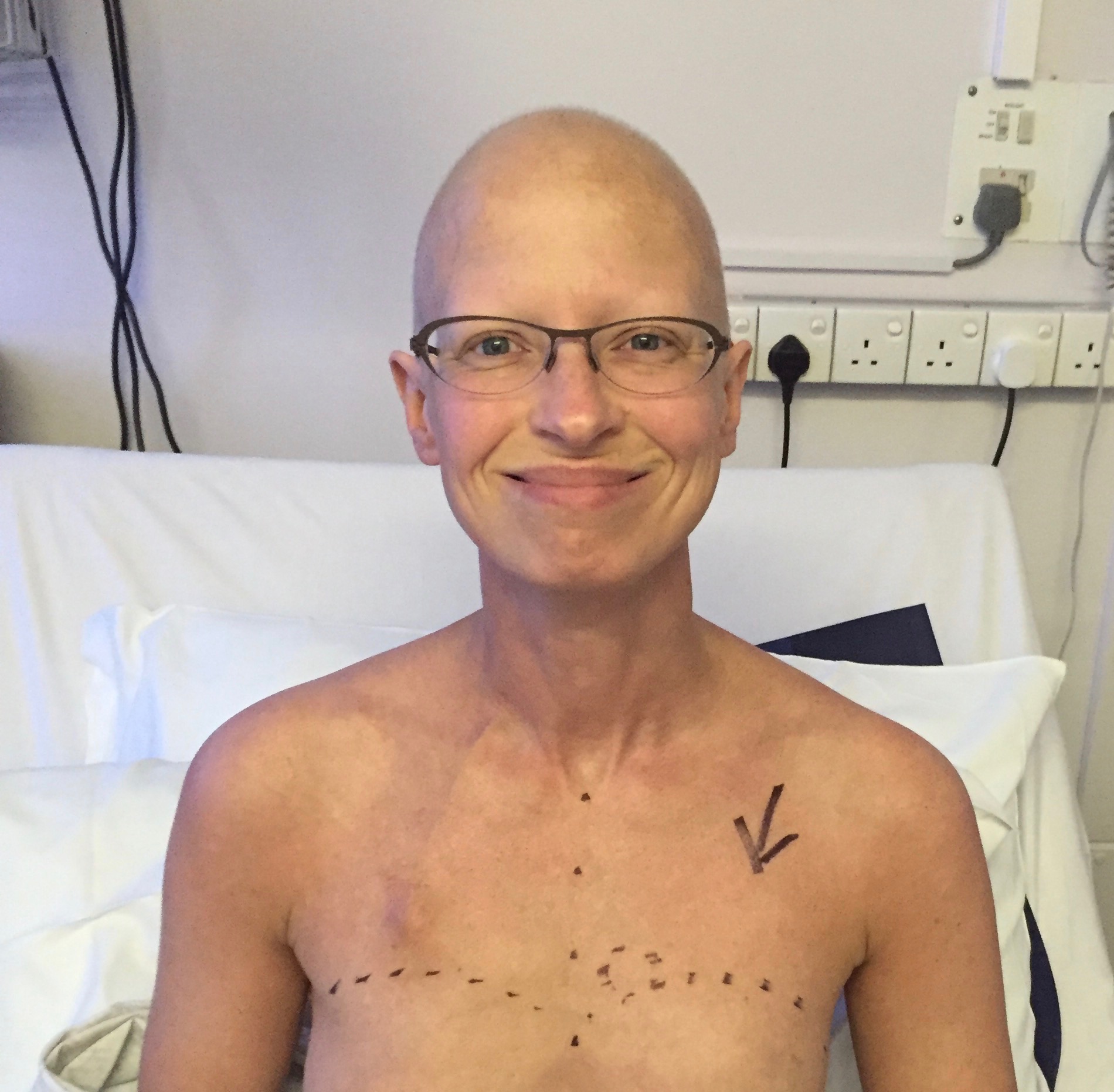
I always tell my patients that I go through 20 years’ of training to be able to draw on people with a permanent marker. It’s important to mark the outline of the breast base, and to mark the side with an arrow, so the correct breast is operated on. The sun was just coming up, and Dermot and I were treated to a beautiful sunrise before we left the room.

Nowhere to hide
All too soon it was time to be wheeled down to theatre. I was first on the list. I had to say goodbye to Dermot, which was awful. We were both tearing up, and I felt so sorry for him. He had banned himself from entering theatre whilst I was having my op. I really hoped he could find someone to distract him and give him a hug to pass the time. I found the short journey being pushed along the corridor into theatres really traumatic. I was half naked, in a hospital gown and a heated blanket (Bair Hugger) to keep me warm and reduce the incidence of a wound infection, with my bald head on show, hanging on to my glasses case. And on the way we kept bumping into people I knew. I felt I had to smile and say “Hello”, and acknowledge them, but I really didn’t want anyone to recognise me in such a vulnerable state.
Dermot had to escape to the park next to the hospital, Hardwick Heath. Fortunately he was spotted by Jessica White, one of the consultant physicians, who escorted him round the Heath and distracted him with talk of spaniel puppies, etc. I can’t imagine what it must have been like for him. All I had to do was go to sleep and wake up again.
Count back from 10…
n the anaesthetic room the staff went through the WHO checklist to make sure that I was who I said I was, check my consent form details and the information on my arm and leg bands with my medical notes. I knew that I was in excellent hands, and the theatre team were all people who I have worked, trained, and laughed with, who would find the next few hours rather difficult, since I was their patient. But they were all wonderful, and I’d even made some chocolate cupcakes for them to eat once they’d finished with me. I also knew that no-one else would be allowed to wander into the theatre whilst I was asleep.
My consultant held tightly onto my hand, and the anaesthetist started the infusion. Bloody hell, did it hurt! I was told that some people feel a burning pain in their forearm was it goes in, and I was definitely one of those people. And then I was out for the count. All I remember is the smiling faces of the women in the room with me.
Wakey wake!
I must have woken up in the recovery room, but I don’t remember. Someone had told Dermot, who didn’t want to intrude, so he sent a colleague to check it was OK for him to see me in Recovery. Apparently I was gabbling away as if I was pissed! I do remember waking up in my side room on the ward, just after lunchtime. I was pain-free, and high as a kite. The local anaesthetic block had worked and I felt amazing! Dermot was there when I woke up, and I must have told him that I loved him about ten times.
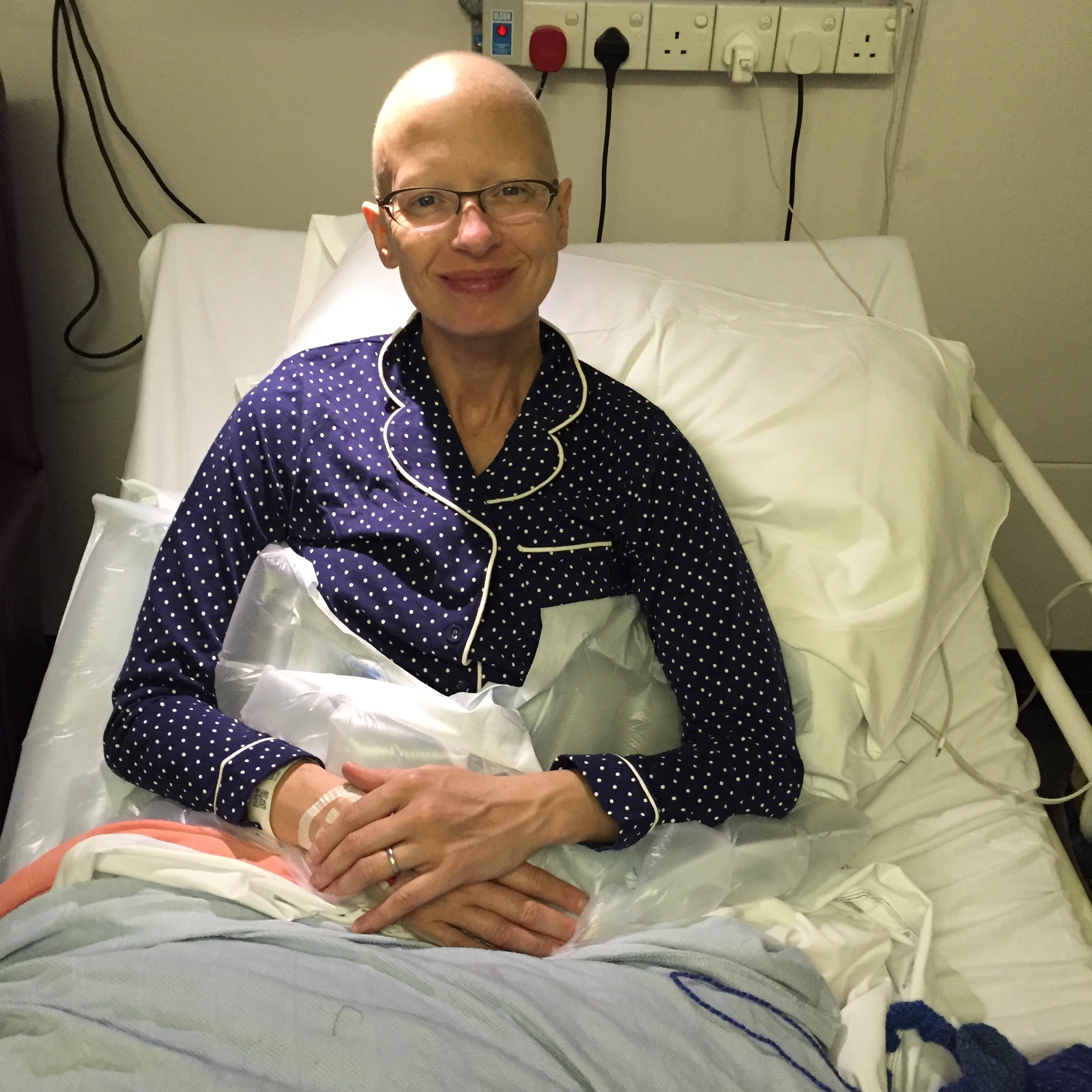
I managed to eat some lunch, and was thrilled that I didn’t feel sick after the anaesthetic. Over the course of the afternoon lots of people came to visit me, who I had worked with when I was a junior doctor at West Suffolk, which was wonderful. The anaesthetist came to check that I was OK, and my surgeon came round at the end of the day. She was happy with how things went, and the drain was draining. I then had a look at my breast – it looked so sorry for itself! I know that the skin normally looks battered and bruised, but it was still a shock to see it with my own eyes. The nipple was a lovely blue colour, and yes, my wee was blue/green too.
I didn’t sleep a wink that afternoon / evening and night. It felt like the operation had given me the equivalent of 12 hours’ sleep and I was too ‘on edge’ to settle down. So I started knitting. I’d been making some Entrelac scarves to keep me occupied, and had brought a ball of wool and my needles with me. It normally takes me 2 days, but I finished one before I was discharged the next day. One of my old friends and theatre nurses (a wonderful “witch” called Janet, one of two, as her witch-in-crime, Tracey, wasn’t working that night) came to see me at night, and we had a right laugh. It was just what I needed, and so lovely to see her after several years.

Come the wee small hours of the morning, the local anaesthetic block was starting to wear off, and I was starting to get very sore. I had been too scared to ask for stronger painkillers. I didn’t know how much pain was normal, and whether I should be asking for something more than paracetamol and ibuprofen. I was also a bit wary of what morphine would taste like, expecting it to be really bitter. I finally asked for some Oramorph, which tasted a bit like cough syrup, and which thankfully took the edge off the pain, and I’m sure helped with the frantic knitting, and I was comfortable again.
Steady as she goes
Moving around the hospital bed was a challenge. I was hooked up to a drip, and had a long drain coming out of my left chest wall, just below where a bra strap sits. I was also under strict orders to have a heated air mattress on top of my chest until the morning. By heating the breast skin it improves the blood flow and helps with healing, but when you’re suffering with hot flushes, the last thing you want is to be under a heated mattress. To say I was a bit sweaty in the morning would be a massive understatement.
A new day
I was starting to get a bit stir crazy by the time morning came, and it was lovely to see Dermot and give him a huge hug. We had to remember not to hug my left side, and he helped me manoeuvre to the bathroom with my drain and drip stand. Then another anaesthetist came to see me, and told me to take regular painkillers and the morphine medicine, and what to stop taking first. I was trying not to have some more oramorph for the pain, because I knew I’d have to wait another 2 hours before I could go home. Trying to push myself up to get out of bed was really sore, and I needed help getting out of my pyjamas and into my bra and shirt. It was also odd touching my reconstructed breast, because it was completely numb. I knew it would be, but it’s quite odd to experience. It feels a bit like when you have an injection at the dentist and think that your cheek is really swollen and puffy, but it’s not.
A bit of ‘me’ time
When my wonderful breast care nurse, Sue, came to see me. I’ve worked with Sue when I was a registrar, so we know each other professionally, and up until now, I’ve been a bit hesitant to let her see the real me, the patient side of Liz, and all my fears and anxieties, especially as she knows my husband as well. But on the morning following surgery, she was amazing. I could suddenly let my professional guard down, and tell her how I was really feeling. It was a huge, and much-needed release.
She gave me instructions on how to look after my drain, with a chart to measure the volume every day. It would stay in for 10 days in total. She then went through the very important arm physiotherapy exercises. I had to do them three times a day, to gradually get the range of movement in my shoulder back to normal. In my own hospital, the women are seen pre-op by a physiotherapist, and they are brought back to a physio group in six weeks to check that no-one has any problems. Some of my patients have found this really useful, mainly because they get to speak to other women who have had the op at the same time as them, and they form their own support network. I never thought I would want a network like this, because I’m not a normal patient and would hate to be forced into advising or counselling the other women, but I did wonder whether it would be good for me to meet women who are going through what I am. I’ve luckily found my own amazing support network through Twitter and Facebook, but not everyone is so lucky.
I was told that I could shower, but needed Dermot to shower with me, so I wouldn’t get tangled up with the drain, and to make sure that I didn’t get the dressings wet. Finally, I was given my appointment to come back for the post-op results.

Drink!
The last person to see me was my surgeon, who was thrilled with the results, as was I. She had done a bloody good job. I was told that I have to avoid heavy lifting for a month. I tell my patients to use the time before their surgery to train their partners and children to cook / clean / vacuum, as the women won’t be able to lift anything heavy for 2 weeks to 5 years, depending on how I’m feeling. The women always laugh, which lightens the mood in the clinic, and I love seeing the look on their partner’s faces. My surgeon told me that I couldn’t drive for a month, I couldn’t run or swim for 2 months, and I wasn’t allowed to lift anything heavier that a full wine glass. I think I love her!
Dermot gently ushered me out to the car, and we were on our way home. I had completed the bike leg of my cancer triathlon without getting a puncture or a penalty for drafting. All that was left was the run, and done!